An Evolutionary Explanation on Why Natural Immunity is Vastly Superior
The Shape of the Adaptive Landscape of the Virus Explains Why Those Who Survive Infection Should Be Left Alone
SARS-CoV-2 uses all of the weapons it has in its arsenal. Why aren’t we?
I have been waiting for some time to write this article, in part because it involves complex ideas from evolutionary theory that most people will have little reasons to immediately understand, and in part due to the need for data to emerge to determine whether the predictions supported by evolutionary biology would bear out.
I also hoped for definitive evidence such as whistleblowers or results from FOIA on the biasing of case rates from the vaccinated and unvaccinated in the US. More on that another day.
There is now little doubt that SARS-CoV-2 vaccination is causing vaccine-induced immune escape. The data in support of the evolutionary escape of the virus from the vaccine are coming in from all over - especially from Israel, the country whose population was sold to Pfizer as an experimentation population for widespread vaccination.
In this Rapid Communication on data from Israel, the authors write:
“(These data challenge) the assumption that high universal vaccination rates will lead to herd immunity and prevent COVID-19 outbreaks. This was probably true for the wild-type SARS-CoV-2 virus, but in the outbreak described here, 96.2% of the exposed population was vaccinated. Infection advanced rapidly (many cases became symptomatic within 2 days of exposure), and viral load was high.”
Counts of Cases, Hospitalizations and Deaths (CHDs) Are Biased in the US
A new study from Yale University shows that the vaccinated can indeed develop severe COVID-19. The authors of that study found that more than a quarter of fully vaccinated patients admitted to the hospital with SARS-CoV-2 were severely or critically ill with COVID-19. However, and importantly, they did not consider people who had received both doses “vaccinated” unless they developed first symptoms or tested positive 14 days following the second dose of the two-dose vaccines, or after seven days of the single-dose vaccine.
The importance of not counting the recently exposed as “vaccinated” as a confounding factor in all analyses of breakthrough cases, hospitalizations and deaths (CHDs) cannot be understated: it biased Moderna’s first efficacy calculations by nearly a third (95% if you exclude people who got COVID-19 before they could be given the second dose; 75% if you include everyone).
The fact that CDC is willing to sequence cases that have a PCR cycle threshold > 40 if they are unvaccinated, but only “scrutinize” and report cases of COVID-19 if their cycle thresholds are <28 AND the patient is hospitalized or dead means a systematic bias exists in what CDC considers “breakthrough cases” (in fact, there are two sets of data, one up to June, 2021 and one thereafter).
The Yale University publication is peppered notably with the usual caveats on the “rarity” of severe COVID-19 among the vaccinated, betraying either undue optimism for technology to stay ahead of SARS-CoV-2 evolution, or a misunderstanding of the fact that rare genotypes can sweep to fixation in a population in a short amount of time in a “selective sweep”, meaning that if the pathogenicity of the virus is related to escape of specific neutralizing antibodies, many if not most vaccinees might, right now, be primed to be at risk of enhanced disease from SARS-CoV-2 infection compared to the unvaccinated or the naturally immune.
COVID-19 New Case Rates Higher in Vaccinated Countries
In an analysis published last month (9/10/2021), I reported that the Our World in Data (OWID) data shows that the higher the vaccination coverage in a country, the higher the new case rates (See: “Do OWID Data Show That Countries with Higher Vaccination Rates Have Higher Numbers of New Cases of COVID-19?”). I reproduce the figure from that analysis here.
It is not a given that the data from the US reporting higher COVID-19 cases in the US is at all reliable, which brings us back to data that appears to be most reliable: Israel (as described above), and Barnstable, County, Massachusetts.
Barnstable County Data Show Vaccine Effective is Zero or Negative
CDC reported that in July 2021, in Barnstable County, Massachusetts, 74% of cases were fully vaccinated. They found the Delta variant in 90% of patients. Importantly, this report showed the Cycle threshold distributions for the vaccinated and the unvaccinated - and found they were similar among specimens from patients who were fully vaccinated. This means there was not a diagnostic-based selection bias in the groups studied. One reason the study found this result was that they defined their groups as individuals who developed COVID-19 within 14 days of exposure vs those who did so 14 days or more after exposure. In other words, they did it right.
This report caused CDC Rochelle Walensky to issue a warning that the vaccinated should still mask, socially distance and otherwise presume that they could still contract and spread SARS-CoV-2. To many who were vaccinated, this felt like betrayal: Fauci and the CDC had promised a return to normal in as a trade for people taking on vaccine risk. Their promise has de-materialized, and Fauci now thinks we’re not going to have Christmas.
Why Natural Immunity is So Much Better Than Artificial Immunity
In my April 2020 analysis which introduced the world to the idea of #PathogenicPriming, I found a total of 54 immunogenic epitopes across all of the SARS-CoV-2 proteins. Nearly all of these epitopes had similarity to human proteins - that is, they had the capacity to induce reactogenic immunity, potentially leading to autoimmunity. Since that publication, the results were validated by researchers at Harvard University and elsewhere; the autoimmune risk associated with SARS-CoV-2 epitopes, including epitopes in the spike protein, has been laboratory-validated, and studied extensively and the number has been expanded to 79 (See Pubmed1 and Pubmed2).
By my estimation, in the spike-protein-only vaccines, all of the humoral response, that is, the adaptive immunity response, is mounted against a maximum of 5 epitopes. It’s not just that the human immune system primed to focus on the original SARS-CoV-2 spike protein will not be able to protect against variants that emerge and escape the vaccine-induced humoral response; it’s also that the vaccines themselves provide selection pressure against a very small part of a very small protein. In other words, when mutations in the spike protein arise, the act of vaccination itself will cause the emergence of - specifically the increase in frequency of - variants for which the vaccine is useless.
That’s simple Darwinian natural selection, and the epidemiologists who blame new breakthrough cases on “the variant” should stop and consider a root-cause analysis: whatever caused the variants to emerge (i.e., spread) also ultimately caused the breakthrough cases. The variant is a penultimate causal factor.
The Complex N-Dimensional Adaptive Landscape of Natural Immunity
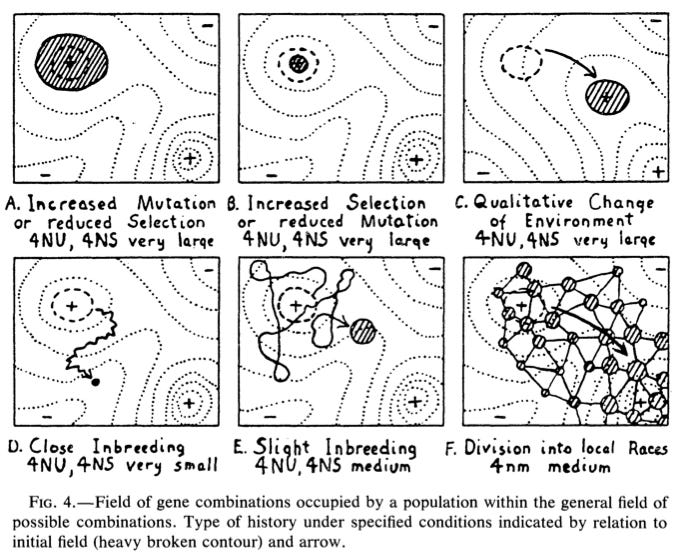
Adaptive evolution was envisioned by Sewall Wright as occurring on a complex N-dimensional adaptive landscape that maps the fitness of an organism to its environment. As the species moves through time, adaptation of an evolving species to an environment is seen as movement across the adaptive landscape of fitness peaks and valleys, with peaks representing moments in time when the species (or individuals in a species) find themselves well-adapted with high survival and reproduction. Valleys represent moments in time in which the species is suffering high mortality or low reproductive output due to a lack of fitness in all, many, or most individuals not well-adapted to the environment in which they find themselves.
The reason why Sewall Wright’s adaptive landscape concept is so impressive is that he published it in 1931 and 1932 - and it was decades ahead of his contemporaries in its scope and ability to capture all of the aspects of evolutionary biology understood at the time.
Figure 4 from Wright (1932, Proc. VI Intern. Cojngr. Genet. 1:356-366), image taken from (http://pleiotropy.fieldofscience.com/2014/01/sewall-wrights-last-paper.html)
Selection of a Single Trait
The spike protein represents, from a phenotypic perspective, a single trait. The viruses uses the spike to enter cells via the ACE2 receptor. There is some evidence it may also enter cells via other receptors, but not nearly as well. One might think that natural selection would favor viruses that could evolve new ways of entering cells, expanding the number of entry points, and diversifying the number of types of cells the virus can enter. It is intuitive that this would lead to higher viremia, but this leads to more severe disease, increasing the likelihood of death.
Factors that would lead to higher reproduction and survival of SARS-CoV-2 therefore actually would include traits that cause decreased viremia, but could only decrease it to a point: from the virus’ evolutionary view, too low viremia means insufficient viremia, leading to reduced transmission.
There is, therefore, counter-balancing selection on lethality via the death and illness in individuals infected with SARS-CoV-2 virus. It is very well understood in virology and parasitology that unsuccessful pathogens kill their hosts; successful pathogens evolve means of surviving via sufficient transmission, but low lethality.
The Humoral Realm: Selection Against Vaccine Neutralizing Antibody Binding Capacity and Waning Immunity
An analysis published in April 2021 warned that immune escape of the receptor binding domain (RBD) of the spike protein (See: “Risk of rapid evolutionary escape from biomedical interventions targeting SARS-CoV-2 spike protein”):
“Our modeling suggests that SARS-CoV-2 mutants with one or two mildly deleterious mutations are expected to exist in high numbers due to neutral genetic variation, and consequently resistance to vaccines or other prophylactics that rely on one or two antibodies for protection can develop quickly -and repeatedly- under positive selection. Predicted resistance timelines are comparable to those of the decay kinetics of nAbs raised against vaccinal or natural antigens, raising a second potential mechanism for loss of immunity in the population.”
Here’s an image of a viral population evolving in a simple environment with selection on a single trait: escape from vaccine neutralizing antibodies. At first, the virus has low fitness due to vaccine-derived antibodies against the spike protein Then, as variants of the virus emerge that escape those antibodies, the virus becomes increasingly fit to replicate in people with antibodies against the spike protein.
Evidence of vaccine escape was described in June 2021 as “emerging” (See “SARS-CoV-2 variants, spike mutations and immune escape”). In an extensive analysis of evidence of adaptive evolution in the spike protein among variants, the authors of that study concluded
“There is now clear evidence of the changing antigenicity of the SARS-CoV-2 spike protein and of the amino acid changes that affect antibody neutralization.”
The concept that single-antigen targeting vaccine-induced humoral immunity might not be able to confer long-lasting immunity against a single antigen source from SAR-CoV-2 has been decried in public presentations by vaccinologist Gregory Poland, who warned against such a design in 2020 (See "Tortoises, hares, and vaccines: A cautionary note for SARS-CoV-2 vaccine development").
Why Natural Immunity is Vastly Superior to Vaccination Immunity
There are a number of reasons why those who survive SARS-CoV-2 infection can expect to have longer-lasting immunity than those who have received vaccines, especially for the spike-protein-only vaccines. First, and most importantly, the spike protein has fewer immunogenic epitopes than the entire SARS-CoV-2 virus. These epitopes provide a diversity of nAbs and a diversity of memory B- and T-cells. Therefore, if immunity from infection conferred by the spike protein epitopes fails, those with prior infection will have redundant, back-up immunity. As I reported in April 2020, there were 54 immunogenic epitopes in the original SARS-CoV-2 proteome. That number has been expanded.
As evolutionary pressure against the spike protein pushes it away from being neutralized by vaccine induced antibodies, the virus cannot escape due to the other antibodies. The multiple components that contribute to fitness now make the adaptive landscape highly complex; from the virus’ evolutionary point of view, mutations that confer protection against nAbs that bind the spike protein do not also confer protection against nAbs that bind, for example, the M protein.
Similarly, mutations that confer protection to the virus from nAbs that bind the M protein do not also confer protection to the virus against nAbs that bind the SARS-CoV-2 endoRNAase.
Similarly, mutations that confer protection to the virus from nAbs that bind the endoRNAase do not also confer protection against nAbs that bind the SARS-CoV-2, helicase, leader protein, or matrix protein. This redundancy is really a numbers game: the probability that evolution will be able to co-localize all of the immune escape mutations into a single virion is exceedingly low, and decreases multiplicatively as the number of antigen sources are increased.
This Means Boosters with the Same Viral Protein Will be Ineffective and Massively Wasteful
The entire world seems focused on neutralizing antibodies. In a study of “waning immunity” following SARS-CoV-2 infection, the authors focused primarily on antibodies and suggested that re-infection or vaccination might be expected to produce prolonged immunity by keeping antibody levels up. They found that while nABs declined, that memory T- and B-cells increased and thus their estimate of the durability of immunity is likely conservative. However, the productions of neutralizing antibodies by itself is not a measure of immunity against an evolving virus: high nAbs are expected to be produced even in patients in whom first-round immunity has waned. (See: "Prospects for durable immune control of SARS-CoV-2 and prevention of reinfection").
To boost the immune system to produce more antibodies that do not work is madness.
Those who are vaccinated will simply experience a boost in nAbs against the original SARS-CoV-2 type, not the more recent types like the Delta variant.
How Multiple Epitopes Should Prevent Viruses from Achieving Immune Escape
Imagine you’re a virus (actually a population of viruses), and you’re happily evolving toward an adaptive fitness peak. The closer you get to the peak, the faster you evolve: runaway selection against viruses that are different from you die off due to the nasty neutralizing antibodies from a spike-protein-only antigen vaccine.
You can see the adaptive peak. Soon, you’ll be surrounded by viruses just like you, all capable of infecting every person you run into, vaccinated or not.
You’re just about there… but then you hit a road block. Your types start dying off. Other types are increasing, but they, too don’t seem to be able to get to the top of the fitness peak. What’s going on?
On your march to the peak, other neutralizing antibodies attack you, keeping you from taking the hill.
You and those like you cannot surpass the immunity escape threshold.
The population in which you and your kind are circulating have already had SARS-CoV-2 infections, and they have multiple B- and T-cell epitopes that keep you from surpassing the immune escape threshold.
You? You’re a goner. The patient you are has taken any of a number of off-label treatments, and gets better in 4 days while they rest quietly at home. You’re done.
This is reality, not fantasy.
In a study of immune response to other epitopes across the SARS-CoV-2 proteome, researchers found strong humoral responses to many epitopes SARS-CoV-2 proteins, notably strong in M, S and N proteins as well ORF3 protein (See: “The landscape of antibody binding in SARS-CoV-2 infection”) The paper is a good read, solid data, and has citations from 2004 and 2006 on synergistic immunogenicity from epitopes found among various proteins in SARS.
From an evolutionary standpoint, durable immunity to SARS-CoV-2 is expected to be more resilient and far, far more effective - and last decade - when dozens of types of memory B- and T-cells have been generated, preventing the emergence of types that can surpass the immune escape threshold. Multifactorial approaches to control viremia are also available - and will help reduce viremia in every patient, instead of forcing them to sit at home and incubate new variants (See: Who Are the World's Leading Authorities in COVID-19 Treatments?).
Thank you, Dr. Wright.
James Lyons-Weiler, PhD
10/6/2021
Citations
The landscape of antibody binding in SARS-CoV-2 infection https://journals.plos.org/plosbiology/article?id=10.1371/journal.pbio.3001265
Multiple fitness peaks on the adaptive landscape drive adaptive radiation in the wild https://pubmed.ncbi.nlm.nih.gov/23307743/
“Evolution on the Biophysical Fitness Landscape of an RNA Virus | Molecular Biology and Evolution | Oxford Academic" https://academic.oup.com/mbe/article/35/10/2390/5046249
Wright S (1988). Surfaces of Selective Value Revisited The American Naturalist, 131(1), pp. 115-123, DOI: 10.1086/284777
Wright S (1931). Evolution in Mendelian populations Genetics (16), pp. 97–159





I have worried constantly that creating a one-sided gauntlet to run is the reason we're seeing such higher case rates in more vaccinated nations. It has shocked me not to see more scientists expressing such concerns.
It also feels like the human body, honed over...well, as long as life here has existed, could already be exceeded by technology at this stage. The notion itself suggests a leapfrogging of a lot of technology we would have expected to see work by now, both in and outside of biology.